Surgical Expertise – Corneal Transplant Surgery
For representative surgical cases and illustrative examples of technique,
please visit the Cornea & Transplants Case Studies page,
where curated videos and case descriptions are available.

Overview
Corneal transplant surgery, also known as keratoplasty, is a surgical procedure in which damaged or diseased corneal tissue is replaced with healthy donor tissue to restore clarity and visual function. The cornea is the transparent front window of the eye, and its integrity is essential for focused vision. Transplantation is typically indicated when scarring, dystrophy or other structural abnormalities of the cornea significantly impair vision and cannot be corrected with other medical or optical treatments.
Dr. Ozana Moraru has extensive experience in corneal surgery, including thousands of corneal transplant procedures performed during her clinical practice at Oculus Eye Clinic in Bucharest. Her surgical work includes both penetrating and lamellar corneal transplant techniques, adapted to the specific needs of each patient.
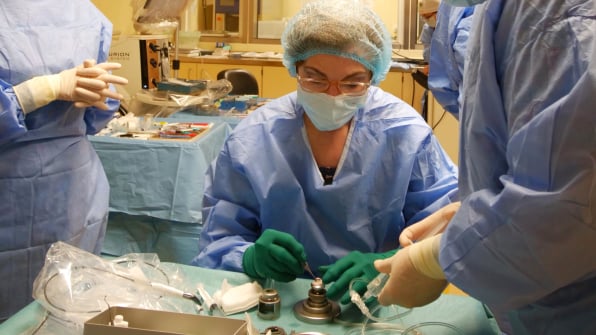
Clinical Approach
Corneal transplantation aims to replace diseased corneal tissue with healthy donor tissue to improve transparency and visual quality. The choice of surgical technique depends on the underlying pathology and the affected layers of the cornea:
Penetrating Keratoplasty (PK) involves full-thickness replacement of the cornea and may be indicated in advanced scarring or irregularities.
Lamellar Keratoplasty (including deep anterior lamellar and endothelial keratoplasty) selectively replaces specific corneal layers, reducing surgical trauma and facilitating rehabilitation.
Dr. Moraru’s approach to corneal transplant surgery emphasizes comprehensive preoperative assessment, accurate tissue selection, and meticulous surgical planning. Her work integrates modern microsurgical techniques and technologies to optimize graft survival, minimize complications and improve visual outcomes in complex cases.
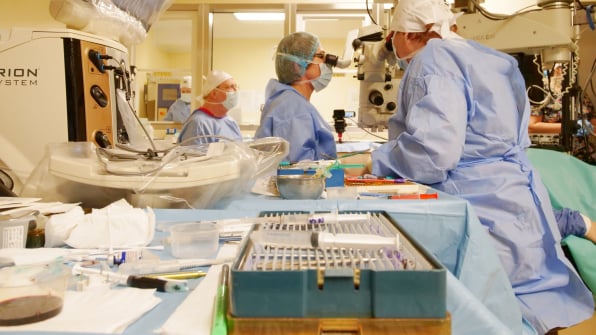
Types of Cases
Dr. Ozana Moraru manages a broad range of corneal conditions that may require transplantation or combined surgical approaches:
Advanced corneal scarring or opacification due to trauma, infections or inflammatory disease;
Endothelial dystrophies and other corneal degenerations;
Keratoconus and other structural abnormalities;
Combined and Complex Procedures in which corneal transplantation is combined with other anterior segment procedures, such as cataract extraction and intraocular lens implantation. These combined approaches require careful surgical sequencing, thorough preoperative planning and the ability to adapt intraoperatively to anatomical and pathological complexity.
Dr. Moraru’s experience in combined anterior segment surgery allows for individualized procedural strategies aimed at maximizing visual outcome while minimizing surgical risk.
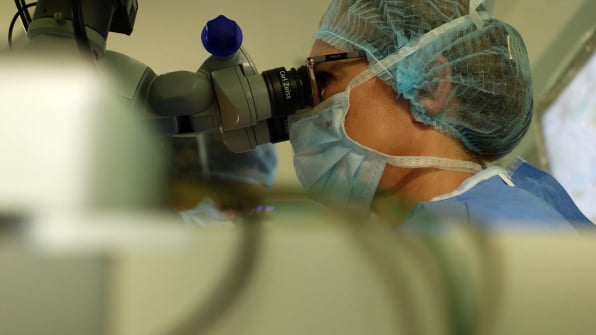
Surgical Technique
Dr. Ozana Moraru’s surgical practice includes both full-thickness and lamellar keratoplasty procedures, selected according to the underlying pathology and anatomical considerations of each case.
Penetrating keratoplasty (PK) involves full-thickness replacement of the cornea and remains indicated in advanced corneal scarring, severe stromal opacification or complex structural irregularities affecting all corneal layers. This technique requires precise donor-host matching, meticulous trephination and careful suturing to ensure graft stability, optical clarity and long-term survival.
Whenever possible, Lamellar Keratoplasty approaches are preferred in order to reduce surgical trauma and improve postoperative recovery.
Deep Anterior Lamellar Keratoplasty (DALK)
is indicated in cases where the corneal pathology is limited to the anterior stroma, with a healthy endothelium. By preserving the patient’s own endothelium, this technique reduces the risk of endothelial rejection and enhances long-term graft survival.
For endothelial dysfunction, Dr. Moraru routinely employs modern posterior lamellar techniques, tailored to the specific clinical context:
Descemet Stripping Automated Endothelial Keratoplasty (DSAEK)
replaces the dysfunctional endothelium and Descemet membrane with a thin donor lamella containing healthy endothelial cells. It offers predictable outcomes, faster visual rehabilitation compared to penetrating keratoplasty, and is well suited for a broad range of endothelial pathologies.
Descemet Membrane Endothelial Keratoplasty (DMEK) involves transplantation of only the Descemet membrane and endothelium, representing the most selective form of corneal transplantation. When feasible, this technique provides superior optical quality, rapid visual recovery and minimal interface disturbance, though it requires advanced surgical expertise and precise intraoperative handling.